Case Report: Executive, Nonprofit Organization
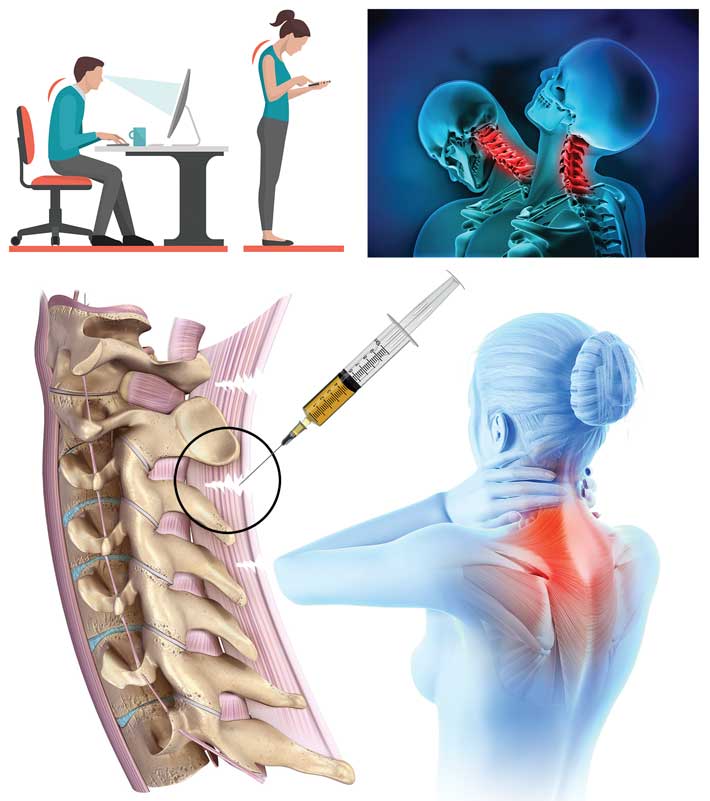
My pain started in 2013 after a severe auto accident that caused a whiplash injury in my upper neck. The pain, headaches, dizziness, and loss of concentration gained momentum in my life gradually, and although I would try to stay engaged in work and home life, it was becoming more difficult. The pain kept me in bed some days, and I was not able to keep work commitments. Simple things like conversing with family and friends were getting to be more difficult.
I saw a spine orthopedic doctor after the accident who treated me with physical therapy, chiropractic, and medications (muscle relaxers, anti-inflammatories) when needed, but when those didn’t work, I received epidural injections for what I was told were cervical herniated discs. The decision to have an epidural was extreme for me; however, I was in pain and could see my symptoms were getting worse with more frequent headaches and dizziness, missing more work, and staying in bed longer. However, unfortunately, the epidurals did not bring me relief. At that point, the spine orthopedic doctor recommended I see a neurologist because I was complaining of dizziness. Upon my first visit, the neurologist requested an EEG and a CT scan, and then prescribed an antidepressant, but I wasn’t depressed (yet). I was in pain! Once the tests were completed, I went back to the neurologist to consult about the results. He said they were negative, and there was nothing abnormal, and he prescribed an anti-seizure medication, Depakote, for migraine headaches. I didn’t return to that doctor or fill the prescription.
I felt I was getting nowhere; my quality of life was no longer what I remembered. I was in bed daily, lying flat to relieve the pain in my head and to prevent the dizziness. Somedays, I couldn’t drive myself, and now I was actually becoming depressed. I then heard about Prolotherapy and went for a consultation.
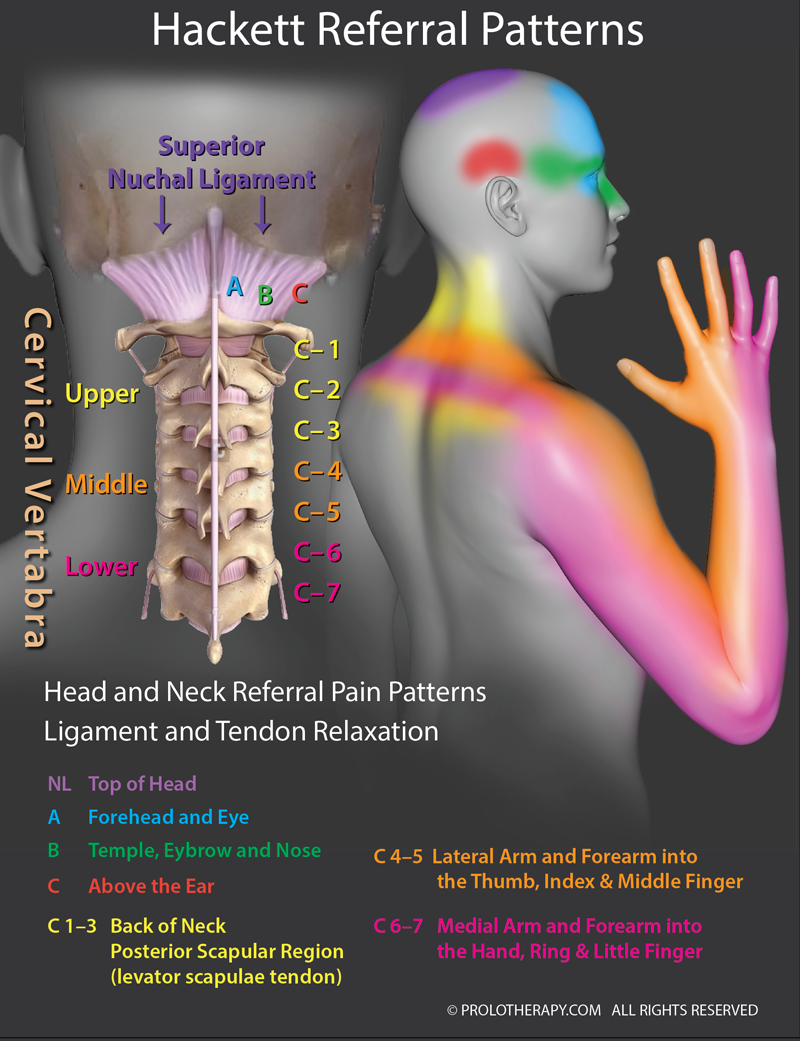
Dr. Alderman listened to me and understood what I was explaining when I told her what had happened to me. She showed me an illustration after my explanation of symptoms that depicted where/how/why this was happening. She explained about Barré-Liéou syndrome, where movement of the stretched ligaments causes pressure on the nerves going to the head, and that this problem does not show up on an MRI or CT because it happens with neck movement, and there is no neck movement during an MRI or CT. It made sense to me that the force of a whiplash could make the ligaments in my upper neck become stretched and weaker, and then normal movement could irritate surrounding nerves, which then could impact my head and focus, I knew at that point that I was going to be receiving the right treatment and embarked on a course of PRP Prolotherapy.
It was a long process, but a necessary process, and it worked! After three treatments, six weeks apart, I was 50 percent better and knew I was on the right track. After six treatments, I was 90 percent improved and back to my prior self. I am again doing the things I love and enjoy. Prolotherapy changed my life forever.
Name withheld for reasons of privacy.